DR. DENNIS HARTLIEB
Blocking out the dark tooth
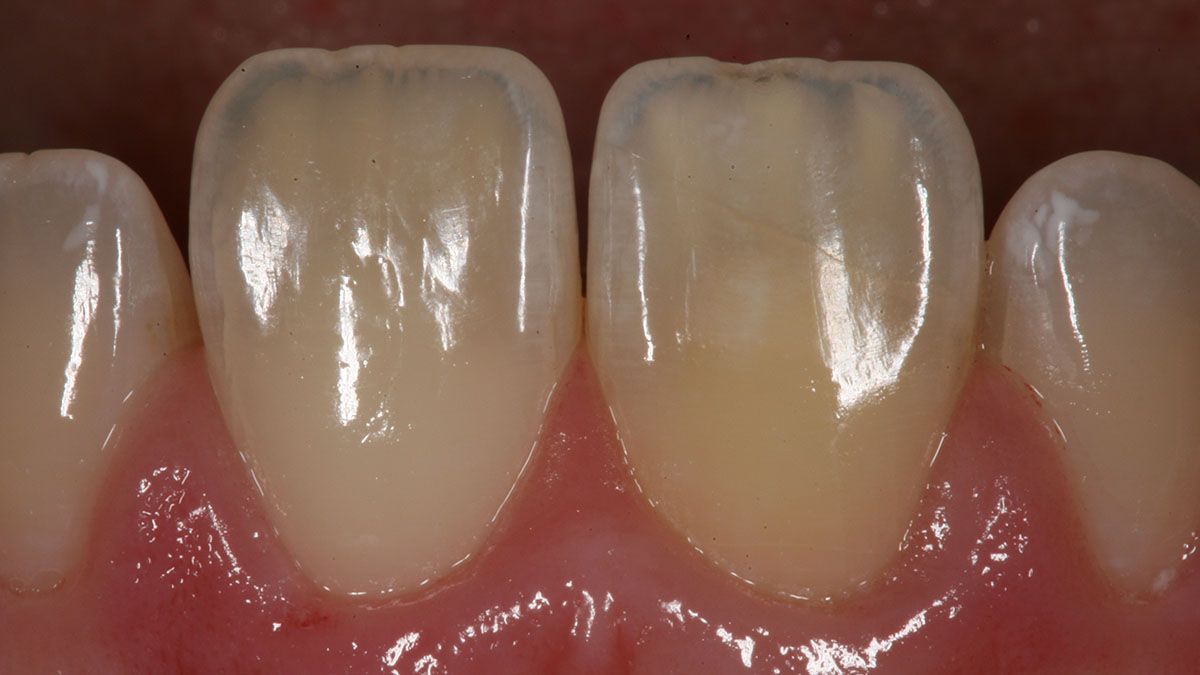
Blocking out the dark tooth
Ok, in your head, name the hardest things to do in cosmetic dentistry. Closing diastemas? Tough, but not the hardest. Prepping tooth #15 in the small mouth patient with the big cheeks and fat tongue? No fun…but not the hardest. Taking accurate final impression of crowns and veneers on an entire arch? Stressful and difficult, but not the worst.
What do I think is the most challenging treatment in cosmetic dentistry? One of three things:
1. Matching the single central incisor with an indirect restoration
2. Replacing the missing anterior tooth, especially when there are bone and soft tissue compromises.
3. Blocking out the dark anterior tooth!
In today’s blog, we are going to limit our conversation to just this one overly stressful dental procedure – blocking out the dark tooth.
The dark tooth comes in several varieties and forms: the traumatized tooth with endodontic treatment, the traumatized tooth that is vital, and the tetracycline stained teeth. When a tooth has been endodontically treated, intracoronal bleaching – i.e. walking bleach, can be utilized with varying degrees of success. However, there are times when the tooth is restored with a post and core build-up restoration and it may be dangerous to remove the post and restorative material in fear of damaging the tooth or fracturing the root. In other cases where the teeth are vital, intracoronal bleaching is not an option. Whitening techniques, such as Kor (in the US) or Enlighten (UK), can lighten tetracycline stained teeth for some individuals, but the timeframe to get to a satisfactory level is extended, and it may be difficult for patients to stay motivated to perform the home bleaching aspect of the treatment.
What do I think is the most challenging treatment in cosmetic dentistry? One of three things:
1. Matching the single central incisor with an indirect restoration
2. Replacing the missing anterior tooth, especially when there are bone and soft tissue compromises.
3. Blocking out the dark anterior tooth!
In today’s blog, we are going to limit our conversation to just this one overly stressful dental procedure – blocking out the dark tooth.
The dark tooth comes in several varieties and forms: the traumatized tooth with endodontic treatment, the traumatized tooth that is vital, and the tetracycline stained teeth. When a tooth has been endodontically treated, intracoronal bleaching – i.e. walking bleach, can be utilized with varying degrees of success. However, there are times when the tooth is restored with a post and core build-up restoration and it may be dangerous to remove the post and restorative material in fear of damaging the tooth or fracturing the root. In other cases where the teeth are vital, intracoronal bleaching is not an option. Whitening techniques, such as Kor (in the US) or Enlighten (UK), can lighten tetracycline stained teeth for some individuals, but the timeframe to get to a satisfactory level is extended, and it may be difficult for patients to stay motivated to perform the home bleaching aspect of the treatment.
If we look at restorative treatment options, things are challenging. Here are today’s options:
1. Full coverage restorations using either zirconia-based crowns or porcelain-fused-to-metal restorations
2. Veneering with a highly opaque porcelain substrate, such as Zirconia
3. Direct resin bonding with composite
Related course: Masking the Dark Tooth with Direct Resin
All three of these options have their advantages and disadvantages. Obviously, full coverage restorations are our least conservative treatment option. Properly executed full crown preparations allow the dental ceramist adequate space to block out the underlying tooth color and still have space for layering porcelain. This is especially true with the more highly opaque zirconia materials that will block out the discoloration leaving enough space for the ceramist to create natural characteristics in the veneering porcelain. Unfortunately, so many of the patients that I have seen with tetracycline staining, have otherwise incredibly healthy teeth free of dental restorations, and they are looking for a treatment option that is not so damaging to their teeth.
Recently, zirconia veneers have been introduced to dentistry. I have yet to place a zirconia veneer (though I have cemented/bonded) many full zirconia crowns and a number of anterior zirconia resin bonded bridges (think single winged Maryland bridge without the metal). The restorations have maintained well, so it is likely that given the proper adhesive protocol and techniques, zirconia veneer restorations should be equally similar in their success rate. But as of now, there is no research that I am familiar with that demonstrates long-term success bonding zirconia veneers.
The other issue, and this where things get really tough when we are dealing with dark teeth, is that the more that we prep the tooth for the restoration, the darker the tooth becomes! That’s right – the enamel is filtering the darkened dentin underneath, and as we remove the enamel to gain restorative space, we make it harder on ourselves to block out the discoloration.
So now that we are prepping deeper to gain space for our restorative material, the more likely we are to having to rely on dentin as our bonding substrate, rather than enamel. In this case, if I am relying on my bond to dentin instead of enamel, my choice of restorative material will always be composite. Why, you ask? For two reasons. Reason #1 – porcelain, especially zirconia, is a very stiff substrate whereas the dentin of the tooth has more flex, especially under function. Composite, in my experience, is better able to ‘bend’ and flex with the tooth structure and I find that the margins maintain better than when I have bonded porcelain to teeth with reduced enamel. The second issue, and this is critical, we must realize that regardless of the material chosen, over time, there will likely be breakdown of the restorative margin interface.
A major advantage of composite over porcelain or zirconia, is its reparability. In cases of margin breakdown, or recession, I can roughen the existing composite and tooth structure, and following proper adhesion procedures, bond new composite to the existing composite covering over the failed margin or the exposed, dark tooth structure. It is my opinion that using composite to veneer dark teeth allows me to manage the inherent challenges of maintaining the restorations long term.
Recently, zirconia veneers have been introduced to dentistry. I have yet to place a zirconia veneer (though I have cemented/bonded) many full zirconia crowns and a number of anterior zirconia resin bonded bridges (think single winged Maryland bridge without the metal). The restorations have maintained well, so it is likely that given the proper adhesive protocol and techniques, zirconia veneer restorations should be equally similar in their success rate. But as of now, there is no research that I am familiar with that demonstrates long-term success bonding zirconia veneers.
The other issue, and this where things get really tough when we are dealing with dark teeth, is that the more that we prep the tooth for the restoration, the darker the tooth becomes! That’s right – the enamel is filtering the darkened dentin underneath, and as we remove the enamel to gain restorative space, we make it harder on ourselves to block out the discoloration.
So now that we are prepping deeper to gain space for our restorative material, the more likely we are to having to rely on dentin as our bonding substrate, rather than enamel. In this case, if I am relying on my bond to dentin instead of enamel, my choice of restorative material will always be composite. Why, you ask? For two reasons. Reason #1 – porcelain, especially zirconia, is a very stiff substrate whereas the dentin of the tooth has more flex, especially under function. Composite, in my experience, is better able to ‘bend’ and flex with the tooth structure and I find that the margins maintain better than when I have bonded porcelain to teeth with reduced enamel. The second issue, and this is critical, we must realize that regardless of the material chosen, over time, there will likely be breakdown of the restorative margin interface.
A major advantage of composite over porcelain or zirconia, is its reparability. In cases of margin breakdown, or recession, I can roughen the existing composite and tooth structure, and following proper adhesion procedures, bond new composite to the existing composite covering over the failed margin or the exposed, dark tooth structure. It is my opinion that using composite to veneer dark teeth allows me to manage the inherent challenges of maintaining the restorations long term.
Application of Pink Opaque
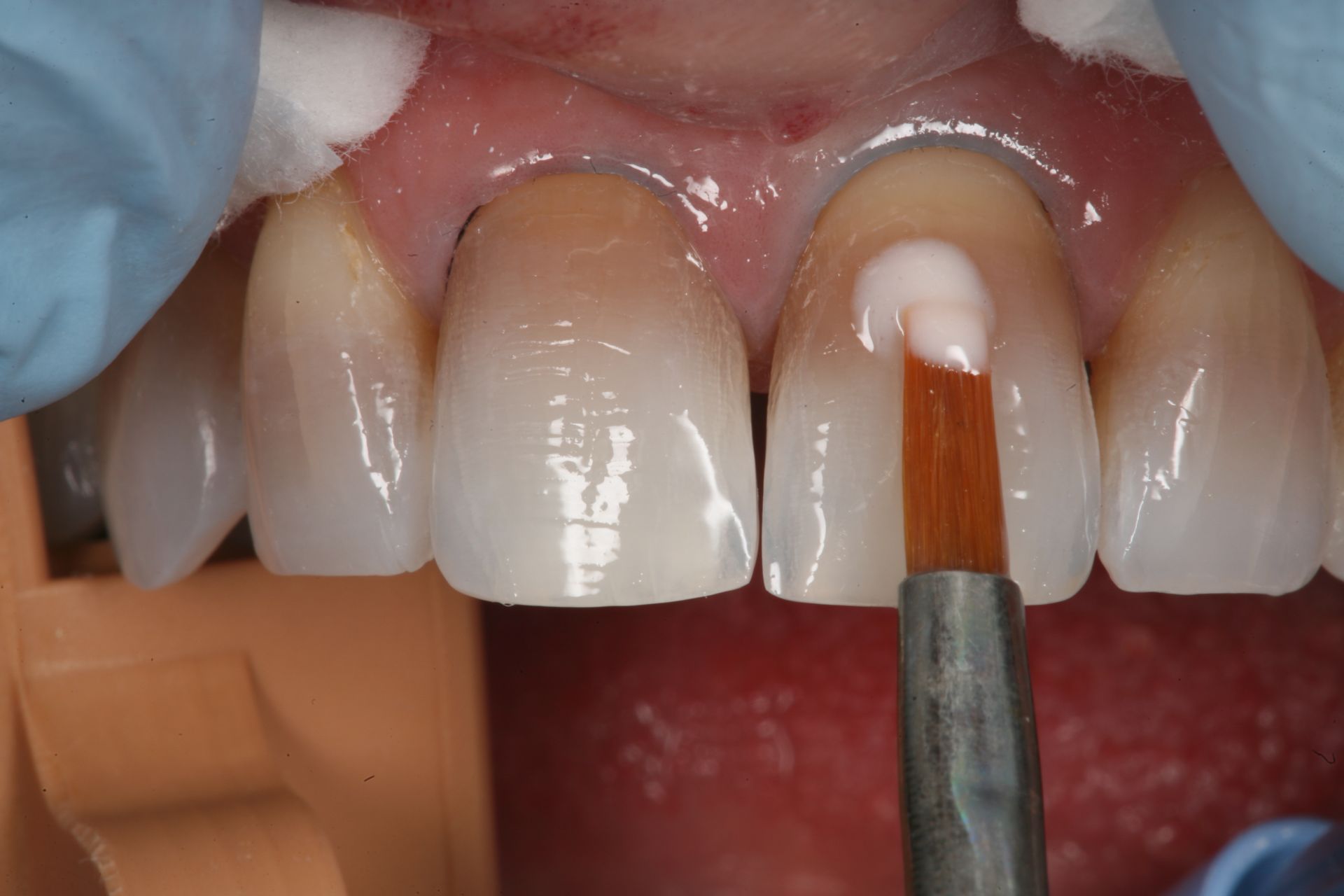
Read also: Blocking out the dark tooth with pink opaque
The other advantage of composite is that it is inherently more opaque than porcelain. We can use this to our advantage when we are working with dark teeth. But it is important to understand the step-by-step workflow when using composite. The first key when blocking out dark teeth is to use a pink opaquer as the first layer of material, after the adhesion technique. Pink opaquer is used to neutralize the dark under color. For clinicians that have tried to use white opaquers, they probably have found that when the white opaquer is used in a thin layer, the value (brightness) is low and the white becomes grey.
Alternatively, when the white is used in a thicker layer, the white will become too opaque in an effort to block out the underlying dark tooth structure, and masking the white with the composite becomes impossible, resulting in an opaque, unnatural restoration. The pink opaque in contrast, when placed in thin layers, raises the value of the restorative surface without over opaquing the tooth. Utilizing pink opaquer as an undersurface allows the dentist to layer traditional composites to create a natural and esthetic final restoration.
Alternatively, when the white is used in a thicker layer, the white will become too opaque in an effort to block out the underlying dark tooth structure, and masking the white with the composite becomes impossible, resulting in an opaque, unnatural restoration. The pink opaque in contrast, when placed in thin layers, raises the value of the restorative surface without over opaquing the tooth. Utilizing pink opaquer as an undersurface allows the dentist to layer traditional composites to create a natural and esthetic final restoration.
Immediate Post-op
I hope that the information on pink opaquer was helpful in understanding its use in pre-opaquing to raise the value of the dark tooth.
Yours for better dentistry,
Yours for better dentistry,
Dennis Hartlieb, DDS, AAACD
DOT Founder
Join 3,000+ dentists who get monthly restorative dentistry tips
Share this page
Latest from our blog

Our vision is to provide online continuing education workshops and mentorship that are comprehensive for dentists learning at all career levels. DOT is developed for dentists that love to learn online.
CONNECT
Materials Included
Light Brown tints, Enamelize, Unfilled Resin Flexidiscs, Flexibuffs 1/2", #1 artist’s brush, Silicone Polishing Points, IPC Off Angle Short Titanium Coated Composite Instrument
Materials Needed, not Included
- Loupes
Follow along
You are Registered
We’re excited to have you join us! You’ll receive email reminders at with the link to join this event.
If you have any questions in the meantime, feel free to reach out to us at dot@dothandson.com—we’re here to help!
Day 1 (8 - 4 pm CST)
-
Erosion and wear – the why and the how
-
Adding length to teeth – when is it safe
-
Opening VDO to compensate for lost tooth structure – where to begin
-
Records visit and key points you need to understand before you start
-
The smile – the 7 strategic points to consider when evaluating the smile
-
Anterior tooth shape, morphology
-
Clinical case review
-
Upper Putty matrix construction
-
Build lingual incisal wall with putty matrix #6 - #11/ Upper anteriors
-
Full contour build-up #6, #7, #8, #9, #10, #11, shape and polish/ Upper anteriors
Day 2 (8 - 2 pm CST)
-
Who – which patients are candidates
-
Why – explaining to patients the value of the prototype
-
How – step-by-step techniques to maximize predictability, efficiency and success
-
Getting to Yes: conversations with patients about esthetic and reconstructive dentistry
-
The ‘Smile Preview’ – techniques to show the possibilities
-
Lower Putty matrix construction
-
Build lingual incisal wall with putty matrix #22 - #27 / lower anteriors
-
Build-up #22 - #27, shape and polish / lower anteriors
-
Build-up lower occlusal posteriors
-
Demonstration of Smile Preview
Upcoming Virtual Workshops
Write your awesome label here.
December 11 & 12, 2025
CPR for the Worn Dentition (16 CE)
Write your awesome label here.
January 29-30, 2026
Porcelain Veneer Cementation Workshop (14 CE)
Write your awesome label here.
March 27, 2026
Esthetic and Functional Success for Diastema Closure (8 CE)
Write your awesome label here.
May 15, 2026
From Break to Beautiful: Flawless Class IV Resin Restorations (8 CE)
Write your awesome label here.
June 19, 2026
Mastering Intraoral Scanners and Digital Workflow for the Dental Team (4 CE)
Write your awesome label here.
September 25, 2026
Veneering the Dark Central Incisor - Conservative Direct and Indirect Restorative Strategies (8 CE)
Write your awesome label here.
October 30, 2026
3D Printing for the Restorative Dentist
Write your awesome label here.
December 11, 2026
Injection Molding Workshop (8 CE)
Write your awesome label here.
Study Club
Join five in-depth virtual meetings held on Thursday evenings throughout the year. Engage in detailed case presentations, discuss curated research articles, and exchange valuable tips with fellow dentists.
-
01/22/2026
-
04/09/2026
-
06/11/2026
-
10/15/2026
-
12/10/2026
Write your awesome label here.
Coffee & Donuts
Kickstart your Friday mornings with informal sessions and discuss patient treatments, practice management, and receive feedback on your cases.
-
01/16/2026
-
02/13/2026
-
03/20/2026
-
04/10/2026
-
05/08/2026
-
06/05/2026
-
08/21/2026
-
10/09/2026
-
11/20/2026
-
12/10/2026
Popular On-Demand Courses
Write your awesome label here.
Injection Moulding Techniques (3 CE)
Simple, predictable, systematic foundation for you to start your journey with injection moulding
Write your awesome label here.
Advanced Techniques in Composite Veneers (6 CE)
Take control of aesthetic cases in your practice, whether you are enhancing smiles with direct resin veneers or creating provisional restorations for indirect cases.
Write your awesome label here.
A Realistic Perspective on Occlusal Appliances (3 CE)
Learn how to design, fabricate, and manage occlusal appliances with confidence through practical guidance and real clinical case examples.
Write your awesome label here.
Bicuspid Veneer and V-Onlay Preparation (3 CE)
Gain expertise in ‘prep-less’ veneers, buccal cusp reduction, and margin placement methods to enhance your clinical outcomes.
Write your awesome label here.
Class IV Composite Restoration – Polychromatic Approach (3 CE)
This on-demand course covers material selection and advanced layering techniques to help you create natural-looking, long-lasting restorations that set you apart.
Write your awesome label here.
EXOCAD: Foundation (2 CE)
Gain the skills to confidently navigate Exocad, build patient cases, and streamline your workflow using time-saving techniques and presets.
Write your awesome label here.
Class II Direct Resin (3 CE)
Master a reliable approach to Class II restorations by learning how to create ideal proximal contacts that enhance both the strength and aesthetics of your work.
